Dr Martin Juneau, M.D., FRCP
Cardiologue, directeur de l'Observatoire de la prévention de l'Institut de Cardiologie de Montréal. Professeur titulaire de clinique, Faculté de médecine de l'Université de Montréal. / Cardiologist and Director of Prevention Watch, Montreal Heart Institute. Clinical Professor, Faculty of Medicine, University of Montreal.
See all articlesOverview
- Voluntary and regular exercise in mice decreases the number of inflammatory leukocytes (white blood cells) in the bloodstream.
- Exercise causes a decrease in leptin (a digestive hormone) secreted by fat cells, which decreases the production of leukocytes by hematopoietic stem and progenitor cells in the bone marrow.
- Cardiac patients who exercised four or more times a week had lower leptin and leukocyte blood levels.
- These results suggest that a sedentary lifestyle contributes to cardiovascular risk through increased production of inflammatory leukocytes.
It is well established that regular exercise has many benefits for cardiovascular health, but the underlying mechanisms have not yet been fully identified and understood. A recent study published in Nature Medicine shows that in mice, voluntary exercise reduces the proliferation of hematopoietic stem and progenitor cells (HSPC), which has the effect of reducing the number of inflammatory leukocytes in the bloodstream. Remember that HSPC cells have the ability to transform into different types of cells that are involved in the immune response (leukocytes, lymphocytes, macrophages, etc.).
A sedentary lifestyle, chronic inflammation and abnormally high white blood cell count (leukocytosis) promote atherosclerosis, which can potentially cause myocardial infarction, stroke or heart failure.
To test whether regular exercise can modulate hematopoiesis, the researchers put mice in cages in the presence (or not for the control group) of an exercise wheel, where they could exercise at their will. Mice use these exercise wheels readily and with great zeal and are therefore not subjected to stress as when they are forced to exercise such as, for example, forced swimming that has already been used in other studies. After six weeks, mice that exercised voluntarily (doing about 20 times more physical activity than sedentary mice) reduced their body weight and increased their food intake.
Analyses have shown that exercise reduced the proliferation of hematopoietic stem and progenitor cells by 34%. The decrease in HSPC through exercise had the effect of reducing the number of inflammatory leukocytes (white blood cells) in the bloodstream. In addition, the mononuclear cells in the bone marrow of mice that exercised were less able to differentiate into granulocytes, macrophages, and pre-B cells. The researchers showed that the mechanism involves a decrease in the production of leptin (a hormone secreted during digestion to regulate fat stores and control the feeling of satiety) in fat tissues. The decrease in leptin in the bloodstream of mice had the effect of increasing the production of factors of quiescence and retention of hematopoietic stem cells in the bone marrow, and consequently of decreasing the number of leukocytes in the bloodstream (see figure below).
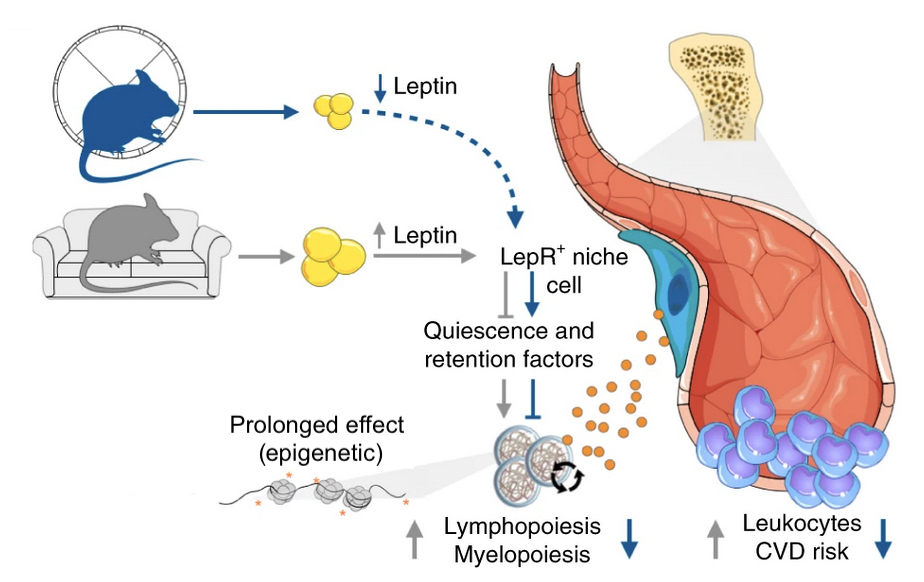
Figure. Schematic summary of the effects of exercise on leukocyte levels and the risk of cardiovascular disease. LepR+: expressing the leptin receptor. Adapted from Frodermann et al., 2019.
Leptin supplementation in mice that exercised (using subcutaneous micropumps) reversed the exercise-induced effects on hematopoiesis, proving that this digestive hormone is involved in this phenomenon.
The exercise wheel was removed from the mouse cage after six weeks. Three weeks later, the effect on leptin production faded, but the effects of exercise on hematopoiesis persisted, i.e. the leukocyte levels of exercise mice were still lower than that of sedentary mice. There is therefore a “memory” of the exercise, which was related to epigenetic changes, i.e. to a difference in the expression of certain genes without alteration of their DNA sequence.
A reduction in leukocyte levels in the blood can lead to an increased risk of infection, as has already been observed for high-intensity exercise. The researchers wanted to see if this was the case with the mice in their study. A component of the cell wall of bacteria (lipopolysaccharide) was injected into the stomachs of mice to induce an inflammatory response. The mice responded quickly by increasing the number of HSPC and defence cells (neutrophils, monocytes, B lymphocytes, T-cells) in the blood and at the site of infection. Mice who exercised reacted more than sedentary mice to lipopolysaccharide injection and had a lower mortality rate when real sepsis was provoked. It is therefore clear that regular voluntary exercise in mice does not decrease the emergency immune response to infection.
The researchers then wanted to find out if the decrease in leukocytes caused by exercise could reduce atherosclerosis and inflammation of atherosclerotic plaques. To do this they used a “knockout” mouse line in which the gene encoding apolipoprotein E was inactivated (Apoe–/–). This protein carries lipids into the blood and is essential for their elimination. Inactivation of the Apoe gene causes hypercholesterolemia and atherosclerosis in mice. Apoe–/– mice that developed atherosclerosis were placed in cages containing an exercise wheel, which led to a decrease in leptin levels, a decrease in leukocytes, and a decrease in plaque size. The same beneficial effects of exercise on atherosclerosis were observed in a mouse line in which the gene encoding the leptin receptor was inactivated specifically at the level of stromal cells.
The researchers finally wanted to know if exercise could have beneficial effects on hematopoiesis in patients with cardiovascular disease. To do this, they checked whether there was an association between the amount of exercise and the blood levels of leptin or the number of leukocytes in 4,892 participants of the CANTOS study, who were all recruited after having a heart attack. Participants who exercised four or more times a week had significantly lower leptin blood levels. Another study (Athero-Express Study) also showed a favourable relationship between the amount of exercise and levels of leptin and leukocytes. The results of these two clinical studies, combined with those obtained in mice, indicate that physical activity has beneficial effects on leptin levels and leukocytosis in patients with cardiovascular disease.
This new study suggests that a sedentary lifestyle contributes to cardiovascular risk through an increased production of inflammatory leukocytes, and confirms the idea that physical activity reduces chronic inflammation. Let us recall the main recommendations of the World Health Organization’s (WHO) regarding physical activity for health:
“In order to improve cardiorespiratory and muscular fitness, bone health, reduce the risk of noncommunicable diseases and depression,
- Adults aged 18–64 should do at least 150 minutes of moderate-intensity aerobic physical activity throughout the week or do at least 75 minutes of vigorous-intensity aerobic physical activity throughout the week or an equivalent combination of moderate- and vigorous-intensity activity.
- Aerobic activity should be performed in bouts of at least 10 minutes duration.
- For additional health benefits, adults should increase their moderate-intensity aerobic physical activity to 300 minutes per week, or engage in 150 minutes of vigorous-intensity aerobic physical activity per week, or an equivalent combination of moderate- and vigorous-intensity activity.
- Muscle-strengthening activities should be done involving major muscle groups on 2 or more days a week.”
To learn more about the benefits, quantity and types of exercise, check out these articles:
How much exercise to live longer?
Exercise on an empty stomach to burn more fat
Can regular exercise compensate for long periods spent sitting?
Exercise benefits in cardiovascular disease: beyond attenuation of traditional risk factors
