Dr Martin Juneau, M.D., FRCP
Cardiologue, directeur de l'Observatoire de la prévention de l'Institut de Cardiologie de Montréal. Professeur titulaire de clinique, Faculté de médecine de l'Université de Montréal. / Cardiologist and Director of Prevention Watch, Montreal Heart Institute. Clinical Professor, Faculty of Medicine, University of Montreal.
See all articlesOverview
- 218 healthy and non-obese people were separated into two distinct groups: one control group where people could eat without restrictions and another whose goal was to reduce their caloric intake.
- For two years, the researchers measured variations in several cardiovascular risk factors, including body weight, cholesterol levels, blood pressure and insulin production.
- The results show that a reduction of only 12% in caloric intake (or 300 calories per day) is associated with a significant improvement in all of these risk factors and could therefore represent a simple way to reduce the risk of cardiovascular diseases.
A recent report found that in 2016, 60% of the population of Organisation for Economic Co-operation and Development (OECD) countries were overweight, including 25% who were obese. This is huge, and this trend will likely worsen in the coming years due to the dramatic increase in the incidence of overweight among young people: in Canada, for example, the obesity rate among children aged 5 to 19 increased from 2.7% to 12.3% between 1975 and 2016, plus another 20% of children who are considered “pre-obese” and therefore at high risk of obesity. These statistics are alarming because being overweight, and particularly obese, significantly increases the risk of type 2 diabetes, cardiovascular and respiratory diseases, and several types of cancer. According to the OECD, the current situation is likely to reduce Canadian life expectancy by 3 years by 2050 (confirming the pessimistic scenario envisaged a few years ago by some researchers), with catastrophic economic and social repercussions.
Excess calories
Contrary to popular belief, the high incidence of overweight in the population is not due to lack of exercise. This discourse comes from multinational food companies that seek to promote their high-sugar and high-fat products by suggesting that it is enough to adopt an active lifestyle to counterbalance the caloric intake provided by these products. In fact, studies indicate that it is practically impossible to “burn” the enormous amounts of calories from these processed industrial products and that one therefore cannot compensate for a poor diet simply by being physically active (“you cannot outrun a bad diet,” as the saying goes). In fact, physical activity levels have remained virtually unchanged in the last thirty years in industrialized countries, so a sedentary lifestyle alone cannot explain the phenomenal increase in population waist circumference that has occurred in recent years. Rather, it is the overconsumption of calories, especially those from ultra-processed industrial food, that is largely responsible for the current worldwide obesity epidemic. To avoid gaining extra pounds, the most important thing is to eat less.
Caloric restriction
Several studies suggest that a reduction in caloric intake is associated with several health benefits, especially at the cardiovascular level, as well as an increase in life expectancy. For example, a study of primates (rhesus macaques) showed that a low-calorie diet reduced the incidence of cardiovascular disease in these animals by about half compared to a standard diet. A similar phenomenon has been observed in humans, i.e. people who drastically reduce their caloric intake to about 1200–1900 kcal/day over a 6-year period showed a dramatic improvement in several cardiovascular risk factors (cholesterol, blood pressure, fasting glucose and insulin, inflammation) compared to those who consumed a standard North American diet (2000–3500 kcal/day).
However, this type of severe caloric restriction is very difficult to maintain over long periods of time for most people, and therefore is not really applicable at the population level. In contrast, a recent study suggests that significant improvements in cardiovascular health can also be seen following a much more modest reduction in caloric intake. In this phase 2 clinical study called CALERIE (Comprehensive Assessment of Long-term Effects of Reducing Intake of Energy), the researchers randomly separated 218 healthy and non-obese people aged 21 to 50 (BMI between 22 and 28) into two distinct control groups: in one control group, people could eat without any restrictions (ad libitum), and in the other, the objective was to reduce caloric intake by 25%. Over a two-year period, several cardiovascular risk factors were measured in both groups, including blood pressure, cholesterol levels, C-reactive protein (a marker of inflammation), insulin and metabolic syndrome (estimated by combining waist circumference, blood pressure, fasting glucose levels, and triglycerides and HDL cholesterol levels).
Participants’ follow-up shows that the objective of reducing the caloric intake by 25% in the experimental group could not be achieved, with a reduction half as small (12%), which corresponds on average to 279 fewer calories/day at the end of the first year and 216 fewer calories/day after two years. Nevertheless, although relatively modest, this reduction is associated with an average weight loss of 7.5 kg (or 10% of the initial weight) and a significant improvement in all cardiovascular parameters measured in the study (Figure 1). Conversely, the volunteers of the control group gained on average a little weight (0.1 kg) and showed no improvement in these various parameters.
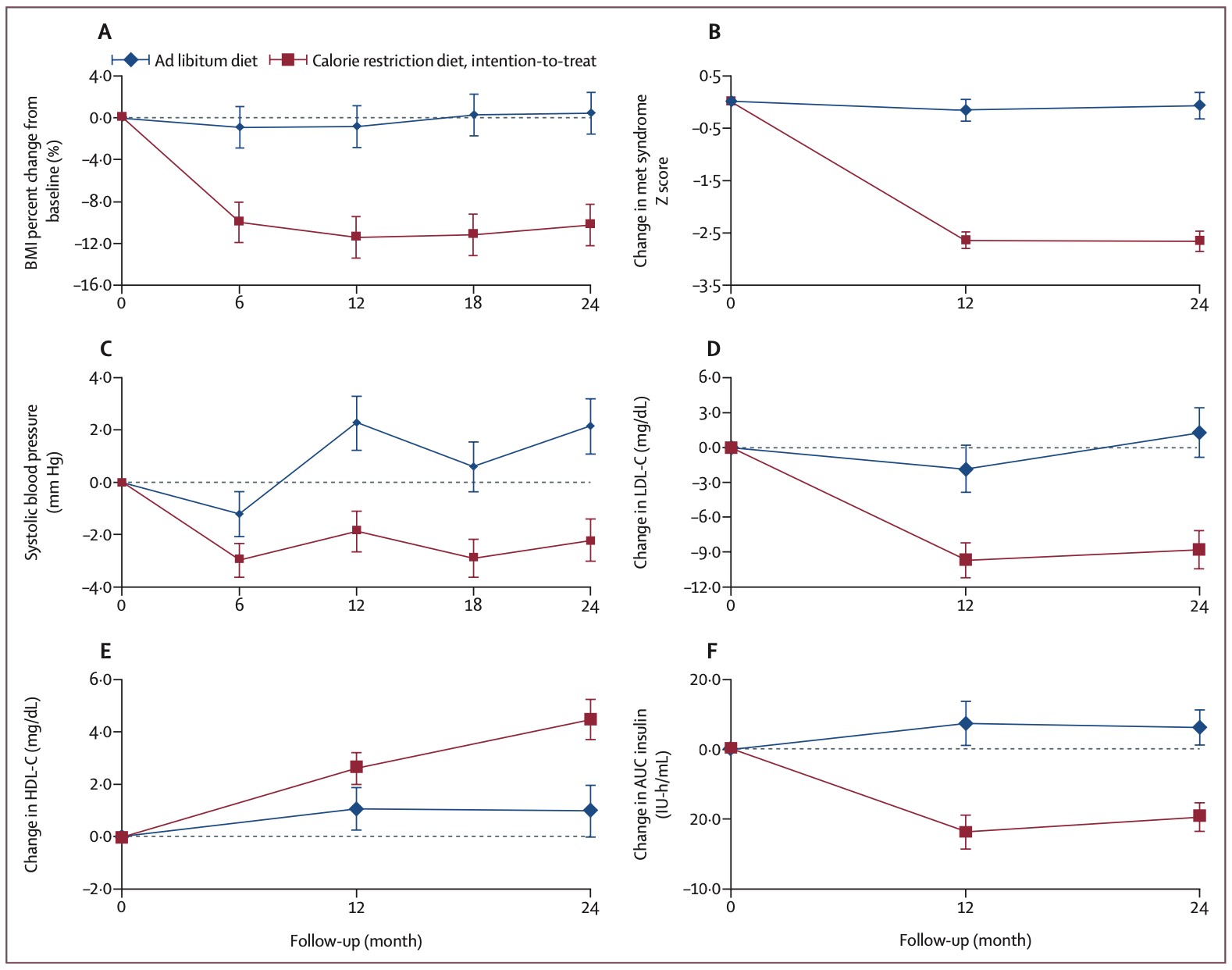
Figure 1. Improvement of several cardiovascular risk factors due to a reduction in caloric intake. From Kraus et al. (2019).
In sum, these results indicate that even in thin and healthy people, a modest reduction in caloric intake (about 300 calories per day, which corresponds to only a slice of pizza) has several positive effects on cardiovascular health. According to the authors, it is likely that these benefits will be even more pronounced in people who are at higher risk of cardiovascular disease due to being overweight. The preventive potential of caloric restriction is therefore immense: according to the OECD report cited earlier, if people in the richest countries, including Canada, reduced their caloric intake by 20%, we could prevent annually 1.1 million cases of cardiovascular disease and save up to $13 billion (USD) each year, a goal that is absolutely impossible to achieve with medication alone.
