Dr Martin Juneau, M.D., FRCP
Cardiologue, directeur de l'Observatoire de la prévention de l'Institut de Cardiologie de Montréal. Professeur titulaire de clinique, Faculté de médecine de l'Université de Montréal. / Cardiologist and Director of Prevention Watch, Montreal Heart Institute. Clinical Professor, Faculty of Medicine, University of Montreal.
See all articlesOverview
- People with cardiovascular disease are more likely to develop the more severe forms of COVID-19, which significantly increases the mortality rate of this disease.
- In addition to being an important risk factor for COVID-19, cardiovascular disease can also be a consequence of SARS-CoV-2 coronavirus infection.
- Patients with severe COVID-19 frequently have heart damage, which increases the severity of the infection and is life threatening.
COVID-19 is a respiratory disease caused by a new virus, the SARS-CoV-2 coronavirus. The COVID-19 epidemic began in December 2019 in Wuhan, Hubei Province, China, and has spread rapidly worldwide with more than 1,360,000 people affected and 75,973 deaths as of April 7, 2020. Although most patients infected with the virus do not have major symptoms, about 15% of them develop a much more severe form of the disease, including severe acute respiratory syndrome that requires mechanical ventilation. This severe form of COVID-19 is particularly dangerous for the elderly: while the mortality rate is around 1% among those aged 50 and under, it rises to 3.6% in those aged 60, to 8% for those aged 70 and up, and to 14.8% for those 80 years and older.
An aggravating factor: Chronic diseases
Data from previous outbreaks caused by coronaviruses similar to SARS-CoV-2 have shown that a large proportion of infected patients are affected by underlying chronic conditions. For example, during the 2002 severe acute respiratory syndrome (SARS) epidemic, the prevalence of type 2 diabetes and preexisting cardiovascular disease was 11 and 8%, respectively, and the presence of either of these chronic conditions was associated with a very large increase (almost 10 times) in the mortality rate. Similarly, in patients infected with Middle East respiratory syndrome coronavirus (MERS-CoV) in 2012 and presenting with severe symptoms, 50% suffered from hypertension and diabetes and up to 30% from heart disease.
The presence of these comorbidities (coexistence in the same patient of two or more diseases) is also observed during the current COVID-19 epidemic. In all the studies carried out to date, a significant proportion of patients were affected by a preexisting chronic condition, the most common being hypertension, type 2 diabetes and cardiovascular disease (Table 1).
| Population | Comorbidities | Source |
|---|---|---|
| 99 infected patients (Wuhan, China) | Cardiovascular disease (40 %) Diabetes (12 %) | Chen et al. (2020) |
| 191 infected patients (Wuhan, China) | Hypertension (30 %) Diabetes (19 %) Cardiovascular disease (8 %) | Zhou et al. (2020) |
| 138 infected patients (Wuhan, China) | Hypertension (31 %) Diabetes (10 %) Cardiovascular disease (15 %) | Wang et al. (2020) |
| 1099 infected patients (China) | Hypertension (15 %) Diabetes (7.4 %) Cardiovascular disease (2.5 %) | Guan et al. (2020) |
| 46,248 infected patients (China, meta-analysis) | Hypertension (17 %) Diabetes (8 %) Cardiovascular disease (5 %) | Yang et al. (2020) |
| 355 deceased patients (Italy) | Hypertension (76 %) Diabetes (36%) Cardiovascular disease (33 %) Atrial fibrillation (25 %) Cancer (20 %) | Instituto Superiore di Sanita (2020) |
In all cases, these chronic conditions are more frequently observed in patients with the more severe forms of COVID-19. For example, a study carried out in Wuhan showed that the proportion of patients with hypertension, type diabetes 2 and cardiovascular disease is almost twice as high in those who have developed a severe form of COVID-19. This contribution of chronic diseases to the burden imposed by COVID-19 seems particularly important in Italy, one of the countries hardest hit by COVID-19: data collected by the country’s health authorities show that 99% of people who have died from the disease had at least one chronic condition such as hypertension (76%), type 2 diabetes (36%), coronary heart disease (33%), atrial fibrillation (25%) or cancer (20%).
The impact of these chronic diseases is considerable, with the mortality rate of COVID-19 increasing by 5 to 10 times compared to people who do not have preexisting conditions (Figure 1).
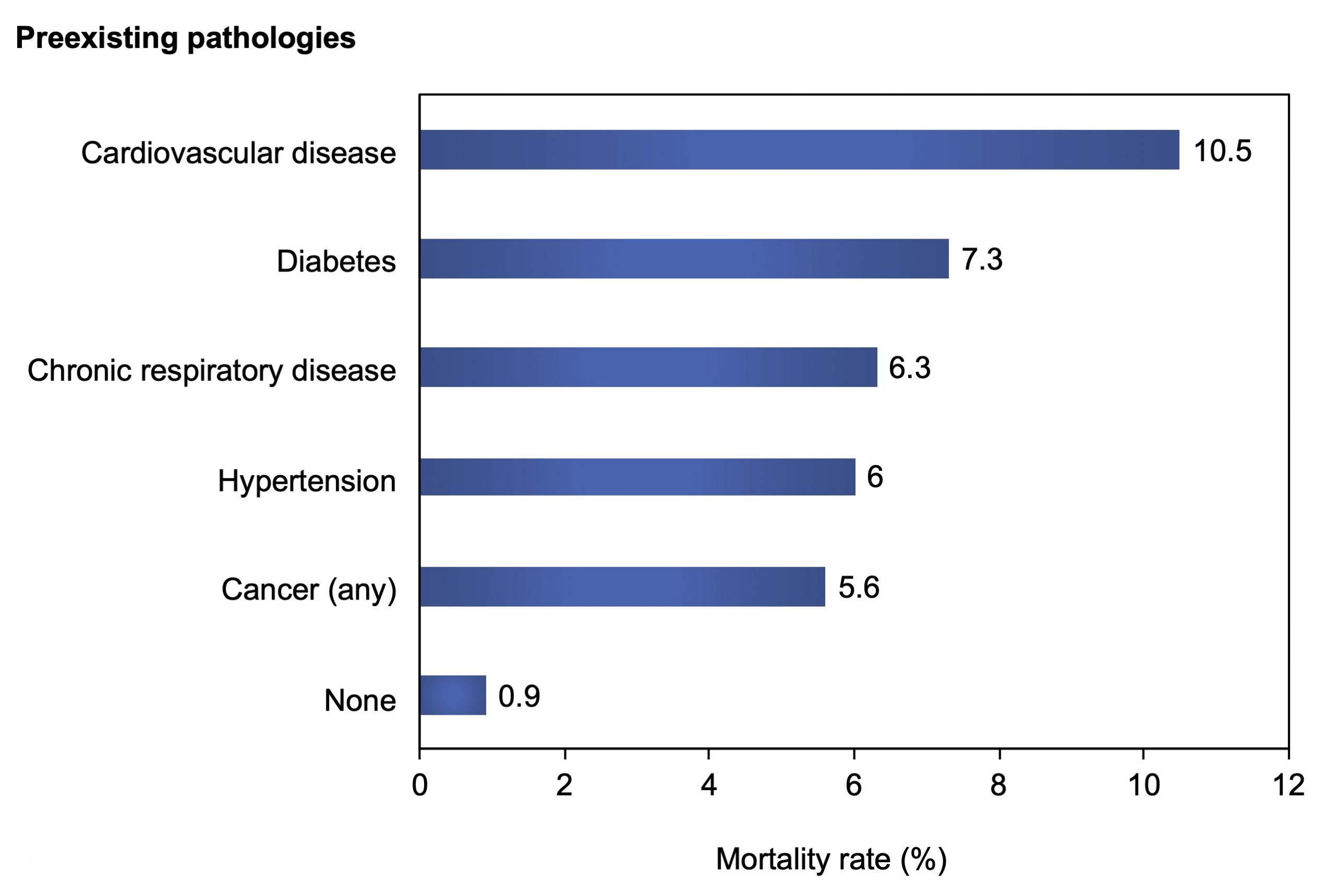
Figure 1. Influence of preexisting chronic conditions on the COVID-19 mortality rate. From: The Novel Coronavirus Pneumonia Emergency Response Epidemiology Team (2020).
People with a chronic condition, including cardiovascular disease, are therefore at much higher risk of developing a severe form of COVID-19, especially if they are older. Consequently, this population must be extra vigilant and avoid interacting with people who may have been in contact with the virus.
Heart damage
In addition to being an important risk factor for COVID-19, cardiovascular disease can also be a consequence of SARS-CoV-2 coronavirus infection. Studies carried out at the beginning of the pandemic observed clinical signs of cardiac injury (elevated blood level of cardiac Troponin I [hs-cTnI], abnormalities of electrocardiograms or cardiac ultrasounds) in 7.2% of infected patients, a proportion that reaches 22% in those affected by severe forms of COVID-19 and who required hospitalization in intensive care. In another study of 138 patients with COVID-19 in Wuhan, 36 patients with severe symptoms treated in intensive care units had significantly higher levels of myocardial injury markers than those not treated in intensive care units. Severe cases of COVID-19 therefore often present complications involving an acute myocardial injury, which seriously complicates the treatment of these patients. It is very likely that these cardiac injuries contribute to the mortality caused by COVID-19, since a study observed hs-cTnI values higher than the 99th percentile (which indicates a myocardial injury) in 46% of patients who had died from the disease, compared to only 1% of survivors. In addition, two recent studies (here and here) have found that the death rate of patients with cardiac injury is much higher than among those without, an increase that can be as high as 10 times in people with a history of cardiovascular disease (Figure 2).
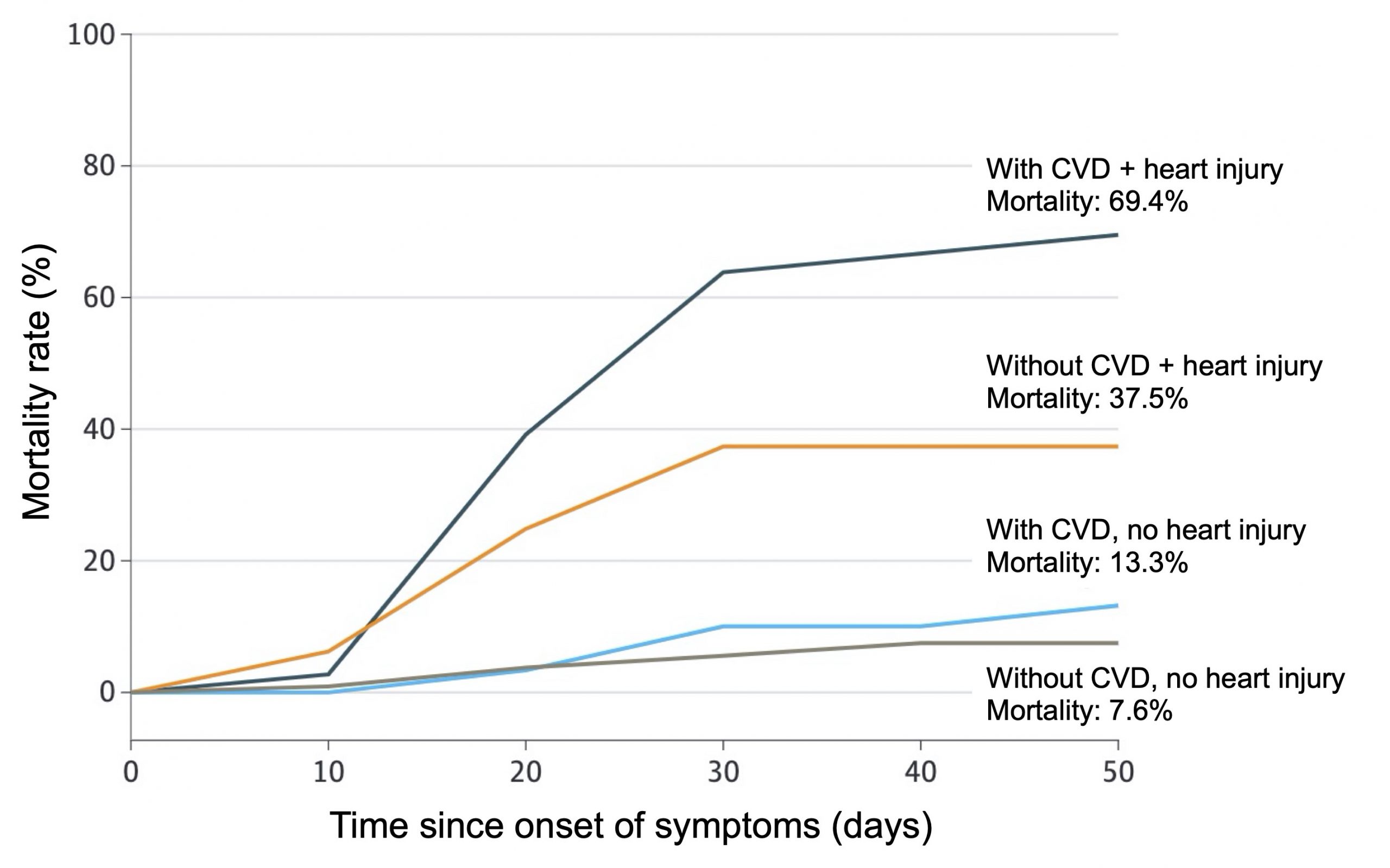
Figure 2. Differences in mortality of patients with COVID-19 depending on the presence of preexisting cardiovascular disease and/or cardiac injury caused by infection. From Guo et al. (2020).
The mechanisms responsible for these heart lesions are very complex and involve several phenomena. On the one hand, poor functioning of the lungs can cause oxygen levels to become insufficient to keep the heart muscle working. This oxygen deficiency is all the more dangerous because the fever caused by the infection increases the body’s metabolism, which increases the workload of the heart. This imbalance between oxygen supply and demand therefore increases the risk of arrhythmia and heart damage.
Another factor involved in heart damage caused by respiratory viruses is what is known as a “cytokine storm”, a phenomenon characterized by an exaggerated inflammatory response following viral infection. The immune system goes berserk and indiscriminately attacks everything in the vicinity, including our own cells, which damages organ function and can increase susceptibility to bacterial infections. The heart is particularly sensitive to this uncontrolled inflammation given its close interaction with the lungs; the oxygenated blood from the lungs reaching the heart has been in direct contact with the foci of infection and therefore necessarily contains a greater concentration of the molecules produced by excess inflammation. When this blood is expelled from the left ventricle to the aorta, a portion of this oxygenated blood is immediately passed to the myocardium to feed the heart cells, with the result that these cells are exposed to abnormally high amounts of inflammatory molecules. An excess of inflammatory molecules can also cause thrombosis (clot formation), which blocks the flow of blood to the heart and causes a heart attack. Indeed, a recent study has shown that high levels of D-dimers, a marker of thrombosis, were associated with a very large increase (18 times) in the risk of mortality from COVID-19.
A clinical study led by Dr. Jean-Claude Tardif, Director of the MHI Research Center, has just been launched to determine whether a reduction in inflammation from viral infection with colchicine, an inexpensive and generally well tolerated anti-inflammatory medication, can prevent the excessive immune response and improve the course of the disease.
It should also be mentioned that in some rare cases, it seems that the heart is the first target of the SARS-CoV-2 virus and that cardiovascular symptoms are the first signs of infection. For example, although the first clinical signs of COVID-19 are usually fever and cough, the National Health Commission of China (NHC) reported that some patients first sought medical attention for heart palpitations and chest tightness rather than respiratory symptoms, but were subsequentlydiagnosed with COVID-19. Recent cases of acute myocarditis caused by COVID-19 in patients with no history of cardiovascular disease have also been recently reported, a phenomenon that had previously been observed for other coronaviruses, including MERS-CoV. A common feature of these viruses is to enter human cells by interacting with the surface protein ACE2 (angiotensin-converting enzyme 2), which is present in large quantities in the lungs, heart and cells of blood vessels. It is therefore possible that the virus uses this receptor to penetrate directly into the cells of the myocardium and cause heart damage. In line with this, it should be noted that analysis of heart tissue from patients who died during the 2002 SARS epidemic revealed the presence of viral genetic material in 35% of the samples. SARS-CoV-2 is very similar (75% identical) to this virus, so it is possible that a similar mechanism is at work.
COVID-19 and hypertension
The interaction of SARS-CoV-2, the virus that causes COVID-19, with the angiotensin-converting enzyme (ACE2) is intriguing, as this enzyme plays a key role in the development of hypertension, and it is precisely hypertensive people who present a more severe form of the infection. Since commonly prescribed antihypertensive drugs cause an increase in the amount of ACE2 on the surface of cells, there have been several texts on social media claiming that these drugs can increase the risk and severity of SARS-CoV-2 infection and should therefore be discontinued. It is important to mention that this hypothesis has no solid scientific basis and that all of the cardiology associations in the world still recommend hypertensive patients continue taking their drugs, whether they are inhibitors of ACE2 (captopril, enalapril, etc.) or angiotensin receptor antagonists (losartan, valsartan, telmisartan, etc.). On the contrary, preclinical studies seem rather to show that antihypertensive drugs could protect against pulmonary complications in patients infected with coronaviruses.
